Premier Orthopaedic Trauma Specialists Announces Merger with Sports Medicine Orthopaedic Institute

We are thrilled to share the exciting news that Sports Medicine Orthopaedic Institute (SMOI) and Premier Orthopaedic Trauma Specialists have officially merged! This collaboration marks a significant step forward in our mission to widen our exceptional orthopedic care to Eastern LA, Orange County, and San Bernadino. It expands access to highly skilled orthopedic surgeons, in-house imaging, and specialized physical therapy services designed to improve our patients’ healthcare experiences.
Premier Ortho Welcomes Chief Operating Officer

Premier Orthopaedic and Trauma Specialists is pleased to announce Armen Hakobyan’s appointment as Chief Operating Officer, effective March 27th, 2024. In this role, he will be responsible for Premier’s overall business operations and the ongoing execution of our strategic vision and values.
Injury to the Ligaments & Meniscus During Sports

The ligaments and the meniscus are structures within and around the knee joint. They and the cartilage of the end of each bone are structures involved in supporting and cushioning the joint. These structures themselves have a limited blood supply and do not necessarily heal well as a result. Bones and muscles, by comparison, tend to have a rich blood supply and may replenish or scar to nearly as good as new with little more than rest and especially with rehabilitation.
How to Make Your Hip Replacement Last Longer
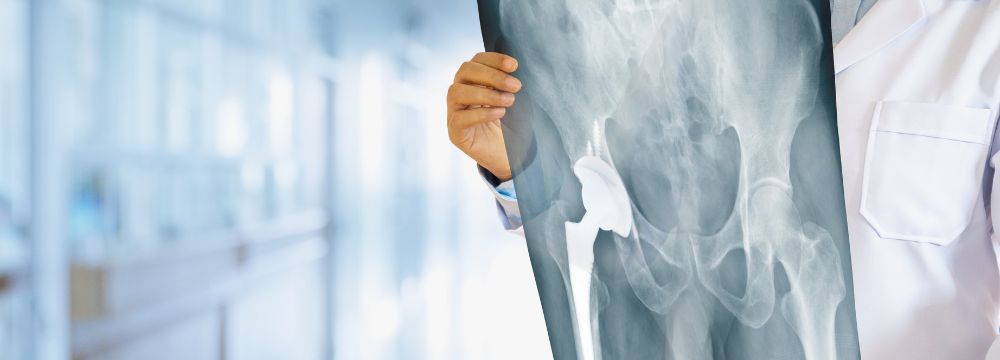
The number of hip replacements over the past ten years has increased dramatically. In fact, The Agency for Healthcare Research and Quality estimates that more than 450,000 of these procedures are performed yearly in the United States. Hip replacements can significantly benefit patients suffering from hip conditions such as degenerative arthritis by dramatically reducing pain, providing increased mobility, and promoting an active lifestyle. So, if you have had a total hip replacement, you may wonder what can make your new hip last longer. The following tips will help prevent the early degradation of your joint replacement.
Improving Knee Stability After an Injury or Knee Replacement

Like many joints throughout our bodies, the knee is a marvel. Even more impressive is that we use and abuse our knees constantly throughout the day, whether with high-impact exercise, injury, or simply placing too much weight on them through lifestyle choices. Yet, for decades our sensitive yet impressively tough cartilage maintains its structure and keeps us pain-free. However, whether due to age, lifestyle choices, or injury, our knees can become damaged and require us to place renewed emphasis on stability to ensure that the knee is not further damaged or that healing can occur properly. This article will discuss how to maintain or improve the knee’s stability. You should always follow these tips even if your knees don’t hurt; prevention is always better and more predictable than treatment.
The Progression From Osteopenia to Osteoporosis: What You Need to Know
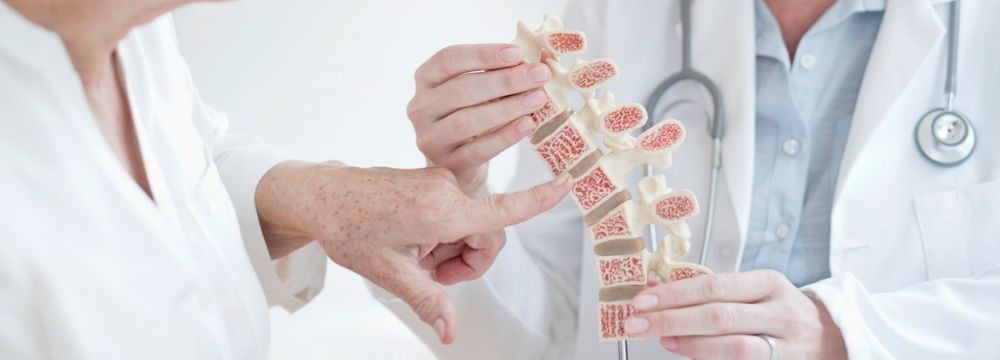
The human skeleton is at the literal core of our bodies. Its most straightforward purpose is infrastructure. Unlike any building, however, this interior scaffold provides support and protection for vital organs and structures, is essential to mobility, serves as a depot for blood cell formation and essential minerals, and even has a purpose as an endocrine organ. The vitality of bone is evidenced in its strength, measurable in density, which can degrade with age.
Home Care For Sports-Related Knee Injuries

When we think of sports injuries, our minds typically go to children’s sports, especially those particularly hard on the knee, like soccer. However, you might be surprised to know how many adults visit our offices and ERs due to significant knee injuries. Of course, as we age, the combination of weakened musculature and the tendency to over-exert, whether to impress or make ourselves feel better, can create a genuinely problematic knee injury situation. The cutting, twisting, turning, and kicking motions can strain the knee. This is true in children and adults alike – especially those who aren’t adequately conditioned or have not warmed up appropriately. Many minor injuries can be treated at home, with an eye toward specific markers that would suggest urgent or even emergent intervention is necessary.
The Right Way to Ride a Peloton or Other Spin Bike

If pandemic-related shutdowns had one benefit to our collective health, it was in the form of introducing exercise equipment into the home. Millions of Americans barred from their gym could bring the gym to them. One of the most popular high-profile companies leading this charge is Peloton, a maker of stationary bikes and treadmills.
However, along with this newfound interest in home exercise, there has been a marked rise in exercise-related injuries, most commonly from overuse. This, of course, stands to reason. You’ve acquired a shiny, new, and typically expensive bike, and you want to use it! Further, the classes that you can take are engaging and fun, making you push ever harder. However, this push can also mean injury if taken too far. Continue reading
Making the Most of Your Downtime After a Joint Replacement

If you were particularly active but are now hobbled by joint issues, the several weeks you need to recover from a joint replacement may be frustrating and driving you out of your mind! Your orthopedic surgeon has already told you that this recovery time is significant for the long-term health of your new joint and longevity. Even so, you may want to accelerate the recovery process. A wrong move could end in further injury. While you should always follow your surgeon’s postoperative instructions, there are a few ways to speed up your recovery and get back to your regular activity faster.
Exercises for Hip, Knee, and Back Pain

Exercise is key to the proper functioning of muscles, bones, tendons, and joints. You may have heard the phrase “motion is lotion” in physical therapy. This is very true. Getting up and being active lubricates the joints, allowing them to function better and work harder for you.
However, chronic pain can keep us sidelined for days, weeks, or months. Even once the pain has subsided or been treated, patients may treat their body too gently with the worry that the pain will return, and they will require additional intervention. However, avoiding exercise only leads to more pain and dysfunction now and in the future.


 ES
ES